Pharmaceutical Traceability in MENA and Africa
Governments across the Middle East, North Africa, and parts of Africa are investing in pharmaceutical traceability systems (national drug traceability systems and supply chain traceability platforms) to strengthen patient safety, improve supply-chain visibility, support recalls, and help combat substandard and falsified medicines. National initiatives in countries such as Saudi Arabia, the UAE, Egypt, and Ethiopia reflect a broader regulatory push aligned with internationally recognized traceability and data standards, including GS1-based serialization approaches (global GS1 traceability standards and serialization compliance frameworks). WHO guidance also recognizes traceability as an important component of stronger regulatory systems for medical products.
Because these systems operate at national scale and affect public-health oversight and healthcare supply chain traceability, governments typically need implementation partners with proven technical capacity, regulatory understanding, and long-term operational reliability. Weak implementation can increase the risk of delays, interoperability problems, added costs, and gaps in supply-chain visibility and transparency. For that reason, vendor selection should be based on demonstrated capability, compliance readiness, and the ability to support sustainable interoperable national deployment aligned with global pharmaceutical traceability standards.
Pharmaceutical Traceability: What Governments Must Consider
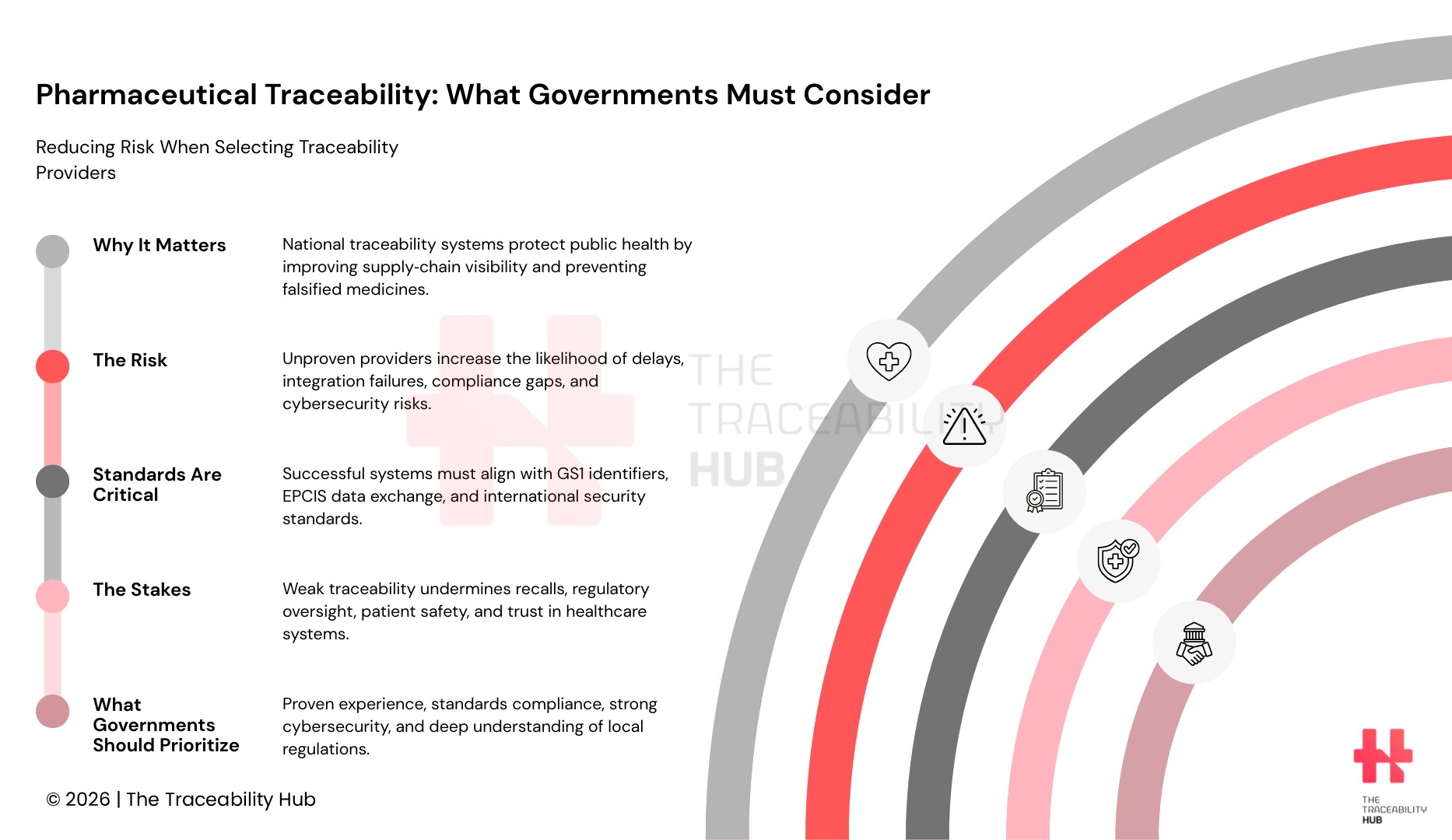
The Risks of Choosing Inexperienced Providers
Limited experience in complex, real-world deployments: Pharmaceutical traceability systems are complex, multi-stakeholder infrastructures (often referred to as national drug tracking systems) that connect manufacturers, distributors, dispensers, and regulators. Because these platforms must function reliably across the supply chain, limited implementation experience can increase the risk of integration problems, rollout delays, and operational inefficiencies, especially in national-scale programs that support recalls, product verification, and regulatory oversight.
Weak alignment with internationally recognized standards: Successful national traceability platforms are typically built on internationally recognized data and identification standards, including GS1 identifiers and EPCIS-based event data sharing (EPCIS traceability frameworks for interoperability). These standards help support interoperability, visibility, and regulatory alignment across supply chain partners. Poor standards implementation can create compliance challenges, reduce interoperability, and complicate participation in regulated trade environments and pharmaceutical serialization ecosystems.
Poor fit with local regulatory and operational requirements: Every national market has its own regulatory structure, operational workflows, and public-sector constraints. Traceability systems must therefore be designed to meet current legal requirements while remaining adaptable as policy and enforcement needs to evolve. Providers without relevant implementation experience may be more likely to underestimate local complexities, creating deployment friction, additional costs, and weaker policy outcomes.
Higher cybersecurity and data-governance risk: National traceability systems process sensitive pharmaceutical supply chain data and regulatory information, making strong cybersecurity and data-governance controls essential. WHO, ISO, and NIST all emphasize the importance of structured risk assessment, information security management, and supply-chain cybersecurity practices in digital systems. Providers should therefore be evaluated on their security architecture, governance processes, and demonstrable compliance with recognized security standards such as ISO/IEC 27001 (information security for pharmaceutical traceability systems).
The Importance of Trustworthy and Experienced Partners
Proven track records support reliable implementation: The deployment of nationwide traceability systems requires vendors with demonstrated experience in comparable regulatory and operational environments. Beyond technical capabilities, experienced providers contribute to implementation of knowledge, scalability expertise, and established best operational practices. This can help reduce deployment risks, improve system reliability, and support more efficient rollout timelines for national drug traceability programs.
Strengthening public health and regulatory oversight: Pharmaceutical traceability platforms can enhance visibility across the pharmaceutical supply chain, supporting product verification, recalls, and regulatory monitoring. When effectively implemented, these systems enable authorities to respond more rapidly to quality incidents and improve data-driven decision-making and strengthen regulatory compliance systems. They can also support audit processes and strengthen coordination between regulatory bodies and supply-chain stakeholders.
Supporting supply-chain integrity and economic resilience: Substandard and falsified medicines pose both public health and economic risks. Pharmaceutical traceability systems can contribute to reducing these risks by improving supply chain transparency, enabling authentication, and strengthening enforcement capabilities. In doing so, they can help protect legitimate market participants and reinforce trust in national healthcare systems.
Facilitating alignment with international requirements: Compliance with internationally recognized traceability and serialization standards (such as GS1 and EPCIS) is often necessary to participate in regulated pharmaceutical markets. By aligning with these standards, countries can improve interoperability, support export readiness for local manufacturers, and position their systems to adapt to evolving global regulatory expectations in pharmaceutical supply chain traceability.
The Real Stakes: Public Health, Security, and Trust
Insufficient visibility throughout pharmaceutical supply chains elevates the likelihood that substandard, falsified, or diverted medicines may reach patients. These risks are extensively documented. According to the World Health Organization, substandard and falsified medical products represent a substantial global public health issue, contributing to treatment failures, heightened antimicrobial resistance, and, in severe instances, patient harm and mortality.
While pharmaceutical traceability systems alone do not eliminate these risks, they are recognized as an important tool to strengthen supply-chain transparency, support product verification systems, and enable faster detection and response to quality incidents. Weak or fragmented drug traceability systems can reduce the ability of authorities to effectively monitor the movement of medicines, manage recalls, and enforce regulatory controls across the pharmaceutical supply chain.
At a national level, these initiatives contribute to strengthening regulatory oversight, improving supply-chain integrity, and reinforcing public trust in healthcare systems. For this reason, the selection of implementation partners should be based on demonstrated capability, reliability, and alignment with long-term public health objectives, rather than on cost considerations alone.
What Governments Should Prioritize
For governments establishing national pharmaceutical traceability programs (or national drug tracking systems), the selection of technology partners is a critical component of successful implementation. These initiatives are increasingly recognized as strategic infrastructure that can strengthen public health systems, enhance regulatory oversight, and contribute to more resilient pharmaceutical supply chains.
Key considerations include:
- Proven implementation experience: Selection processes should prioritize providers with demonstrated experience in delivering national or large-scale traceability pharmaceutical systems, particularly in comparable regulatory environments and serialization programs.
- Alignment with internationally recognized standards: Solutions should align with widely adopted standards such as GS1 identification systems and EPCIS-based data exchange, as well as relevant ISO standards (e.g., ISO/IEC 27001 for information security), to support interoperability and pharmaceutical regulatory compliance.
- Robust cybersecurity and data governance: Providers should demonstrate strong cybersecurity capabilities and established data governance frameworks, in line with recognized international best practices for healthcare and pharmaceutical traceability systems.
- Understanding of local regulatory and operational contexts: Effective implementation requires alignment with national regulatory frameworks, healthcare workflows, enforcement mechanisms, and pharmaceutical supply chain structures, combined with knowledge of international best practices.
Given the public health implications, regulatory importance, and operational complexity of these pharmaceutical traceability systems, governments are encouraged to base partner selection on demonstrated reliability, technical capability, and long-term sustainability.
Coming soon: The Future of Supply Chain Innovation: How AI and Automation Are Changing Everything





